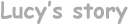
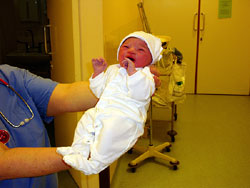
  Lucy
was born on 12th March 2004.
Despite the spikey hair and hairy forehead, she was
perfect! And it was the happiest day of our lives. The
next few weeks and months were very happy as we adjusted
to a new person in our lives. Life couldn’t get
any better. We often wondered why we had left having
kids as late as we did, it was the happiest feeling. Lucy
was born on 12th March 2004.
Despite the spikey hair and hairy forehead, she was
perfect! And it was the happiest day of our lives. The
next few weeks and months were very happy as we adjusted
to a new person in our lives. Life couldn’t get
any better. We often wondered why we had left having
kids as late as we did, it was the happiest feeling.
We went on holiday to France for
2 weeks at the end of September before Lucy started
nursery and Nic went back to work. Our lives started
to change direction from then on after Lucy started
nursery and was exposed to new bugs and infections.
She was very happy at nursery, but had quite a bit of
time off (and also we had quite a bit of time of work).
This didn’t seem out of the ordinary as most kids
suffer virus after virus after starting nursery, especially
at the time of year when the nights are drawing in and
temperature drops. One thing that did occur to us after
a few weeks of this run of sickness was that Lucy didn’t
seem to cope with illness that well and whatever it
was that week that was going round nursery lucy got
it, and got it worse than the others. Croop was a problem
for Lucy and we had a number of visits to A&E throughout
October and November because she was having difficulty
breathing. Whilst this was worrying for us new parents,
we didn’t really consider anything by it, it was
just life with a new child at nursery. Also we noticed
that Lucy’s weight was by now not really progressing
as it should have done and in November was still the
same weight as she was in September before she started
nursery. She was a faddy eater and as soon as she got
ill with a cold or whatever, food and drink went out
of the window. it was a constant source of worry for
us.
 At
the end of November Lucy acquired a really heavy cold.
We were worried as she did seem quite poorly, but thought
as usual she would be crook for a few days and then
back to normal. We decided that I should continue with
plans to go away for the Saturday night to watch a football
match that we’d had tickets for for weeks. The
Saturday night was difficult for Nic, lucy went down
hill and seemed to have breathing difficulties over
night. On my arrival back in Oxford on Sunday we took
her straight to the out of hours GP service and they
referred her straight to A&E as they thought she
had a chest infection and her chest did not sound right.
In A&E they took a chest x-ray and thought it was
clear. They told us she had bronchilitus (as had many
kids in Oxford at that time and A&E had been inundated
that day) but that her blood Oxygen levels were good
(98% approx) and we should keep an eye on her and bring
her back if she got worse. We felt reassured that it
was nothing too “major” and that it would
pass in a few days. Our Sunday night was bad, she At
the end of November Lucy acquired a really heavy cold.
We were worried as she did seem quite poorly, but thought
as usual she would be crook for a few days and then
back to normal. We decided that I should continue with
plans to go away for the Saturday night to watch a football
match that we’d had tickets for for weeks. The
Saturday night was difficult for Nic, lucy went down
hill and seemed to have breathing difficulties over
night. On my arrival back in Oxford on Sunday we took
her straight to the out of hours GP service and they
referred her straight to A&E as they thought she
had a chest infection and her chest did not sound right.
In A&E they took a chest x-ray and thought it was
clear. They told us she had bronchilitus (as had many
kids in Oxford at that time and A&E had been inundated
that day) but that her blood Oxygen levels were good
(98% approx) and we should keep an eye on her and bring
her back if she got worse. We felt reassured that it
was nothing too “major” and that it would
pass in a few days. Our Sunday night was bad, she 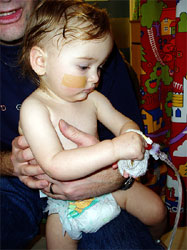 seemed
to get worse and was struggling to breathe overnight,
she spent the night in our bed and neither Nic or I
got a wink of sleep. In the morning she seemed to improve
slightly and so I went off to work as normal. Nic didn’t
work on Mondays so she was at home with Lucy. In the
afternoon I got a call from nic who was clearly worried
about Lucy’s condition as she had deteriorated
again, not feeding, struggling to breathe etc etc. Nic
decided it was best to take her back to A&E for
another check-up. I agreed and said I’d meet her
there. It was a good decision! After we had been in
A&E for about 2 hours (after the senior doctor had
decided that Lucy needed admitting to hospital as her
blood oxygen levels had dropped to about 91% and needed
some help, through Oxygen, to breathe) she took a serious
turn for the worse. Within what seemed like the blink
of an eye her blood oxygen had dropped to below 60%,
her colour had drained completely and her heart was
working overtime to keep her going, she had been rushed
into the Resuscitation room and had 10 to 15 medical
staff buzzing round her. We were told that Lucy was
critically ill and that they were working hard to save
her life. She was being stuck with needles in her hands,
feet, arms getting lines into her to give IV antibiotics
and fluids. It seemed like we had been transported into
our worst nightmare and all we could do was stand and
watch, in a complete state of panic. This situation
went on for about an hour and a half and slowly she
came round. The doctors,
despite not really knowing what was seemed
to get worse and was struggling to breathe overnight,
she spent the night in our bed and neither Nic or I
got a wink of sleep. In the morning she seemed to improve
slightly and so I went off to work as normal. Nic didn’t
work on Mondays so she was at home with Lucy. In the
afternoon I got a call from nic who was clearly worried
about Lucy’s condition as she had deteriorated
again, not feeding, struggling to breathe etc etc. Nic
decided it was best to take her back to A&E for
another check-up. I agreed and said I’d meet her
there. It was a good decision! After we had been in
A&E for about 2 hours (after the senior doctor had
decided that Lucy needed admitting to hospital as her
blood oxygen levels had dropped to about 91% and needed
some help, through Oxygen, to breathe) she took a serious
turn for the worse. Within what seemed like the blink
of an eye her blood oxygen had dropped to below 60%,
her colour had drained completely and her heart was
working overtime to keep her going, she had been rushed
into the Resuscitation room and had 10 to 15 medical
staff buzzing round her. We were told that Lucy was
critically ill and that they were working hard to save
her life. She was being stuck with needles in her hands,
feet, arms getting lines into her to give IV antibiotics
and fluids. It seemed like we had been transported into
our worst nightmare and all we could do was stand and
watch, in a complete state of panic. This situation
went on for about an hour and a half and slowly she
came round. The doctors,
despite not really knowing what was 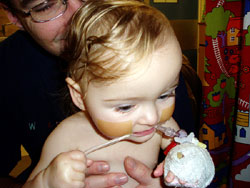 wrong
with her had managed to bring her round but she was
still very poorly and not the Lucy we knew. We were
then sent round to Paediatric ITU where we spent about
3 hours so that they could keep a close eye on her and
ensure she was out of danger. We made it up to ward
4C at about 10pm that Monday evening. Our parents had
been worried sick when I phoned them about 9pm as they
knew Lucy was unwell, and had tried to phone us at home
with no answer, they knew something was wrong. I will
never forget that phone call to my mum, it was very
upsetting. We felt totally traumatised by our experiences
that day. Lucy spent 4 days in hospital, steadily improving
each day. The poor little girl who wasn’t yet
9 months old wondered what was going on. We got her
home on the Friday lunchtime after what had been a difficult
and exhausting week. We reflected on our experiences
a lot over the next few weeks and just didn’t
know why Lucy had become so ill. wrong
with her had managed to bring her round but she was
still very poorly and not the Lucy we knew. We were
then sent round to Paediatric ITU where we spent about
3 hours so that they could keep a close eye on her and
ensure she was out of danger. We made it up to ward
4C at about 10pm that Monday evening. Our parents had
been worried sick when I phoned them about 9pm as they
knew Lucy was unwell, and had tried to phone us at home
with no answer, they knew something was wrong. I will
never forget that phone call to my mum, it was very
upsetting. We felt totally traumatised by our experiences
that day. Lucy spent 4 days in hospital, steadily improving
each day. The poor little girl who wasn’t yet
9 months old wondered what was going on. We got her
home on the Friday lunchtime after what had been a difficult
and exhausting week. We reflected on our experiences
a lot over the next few weeks and just didn’t
know why Lucy had become so ill.
The rest of the winter was difficult
as we lurched from one illness to the next. February
came and saw Lucy admitted to hospital again with a
really bad bout of Gastroenteritis, this time she was
in for 3 days. Lucy’s weight was still about the
same as it had been back in October and her numerous
illnesses kept knocking her back. We were seeing Dieticians
about this but anything we tried didn’t seem to
work.
We went back to outpatients
in mid March for our final follow-up from her bronchilitus/pneumonia
event (just before Lucy’s 1st birthday) where
we expected to be discharged. After a brief chat the
doctor left the room to check something with the Consultant.
The consultant came back in to look at lucy and it was
then a bomb was dropped on us. The doctors thought that
Lucy had an elongated head and no evidence of a “soft
spot” on the top of her head. They thought that
she might have a condition called Craniosynostosis,
but would need to do x-rays of her skull to be sure.
We were in a spin again with no idea of what this condition
was, what it meant, why? when? so many questions buzzing
round our heads with no real answers. We came back in
for x-rays the following week and saw the Consultant
straight afterwards. The diagnosis was confirmed, Lucy
had Saggital Craniosynostosis.
The doctor tried as best she could to explain what it
was and what would be the likely course of events, but
she would be referring us to Mr Wall, Consultant Craniofacial
and Plastic Surgeon at the Radcliffe Infirmary in Oxford.
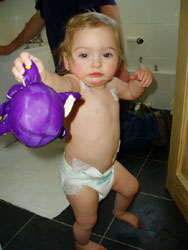
In layman’s terms it meant that Lucy’s saggital
suture line (the centre gap) in the top of her skull
had fused together too early which meant that her skull
was not growing in a uniform way and her head was becoming
overly elongated and a high forehead. It seemed so unfair
on Lucy, who had already been through so much that she
now had to endure more upset and hospital visits. We
were devastated and despite trying for it not to take
the shine of her birthday celebrations, it did, certainly
for us parents anyway.
 We
got an outpatients appointment through with Mr Wall
for early April. He explained in more detail about the
condition and what it meant and broadly what the procedure
would be to rectify the problem. The “good”
news was that the type of synostosis Lucy had was the
most common and was usually non-syndromic ie that there
is usually no other disorders that accompany it and
other than the potential risk of brain damage if the
operation is not undertaken everything else should be
fairly straight forward. (It did become apparent though
that Lucy’s previous health problems may not be
completely unrelated to this condition. It was suggested
to us that whilst they would never know for sure, other
babies/children with this condition have been on the
small side and therefore have tended to be more “sickly”
than other kids. Despite us being devastated by the
news of Lucy’s diagnosis, we did get some positive
thoughts about the fact that we may now be understanding
why Lucy had been hit so hard by fairly minor illnesses
and ailments, that other kids would have just shrugged
off). Mr Wall said they would need to do a CT scan as
soon as possible to ascertain exactly what the situation
was, but in his opinion the operation would need to
be done. Lucy had her CT scan in mid April which meant
a general anaesthetic for her. We saw Mr Wall again
in May with the results of the scan which again reconfirmed
the diagnosis and the need for the operation, although
again there was good news, there was no evidence yet
of intracranial pressure (pressure within the brain
due to a constricted space to grow) which meant the
operation was not mega urgent. For us, once we knew
it needed to be done we just wanted to get on with it,
despite the thought of it scaring the hell out of us! We
got an outpatients appointment through with Mr Wall
for early April. He explained in more detail about the
condition and what it meant and broadly what the procedure
would be to rectify the problem. The “good”
news was that the type of synostosis Lucy had was the
most common and was usually non-syndromic ie that there
is usually no other disorders that accompany it and
other than the potential risk of brain damage if the
operation is not undertaken everything else should be
fairly straight forward. (It did become apparent though
that Lucy’s previous health problems may not be
completely unrelated to this condition. It was suggested
to us that whilst they would never know for sure, other
babies/children with this condition have been on the
small side and therefore have tended to be more “sickly”
than other kids. Despite us being devastated by the
news of Lucy’s diagnosis, we did get some positive
thoughts about the fact that we may now be understanding
why Lucy had been hit so hard by fairly minor illnesses
and ailments, that other kids would have just shrugged
off). Mr Wall said they would need to do a CT scan as
soon as possible to ascertain exactly what the situation
was, but in his opinion the operation would need to
be done. Lucy had her CT scan in mid April which meant
a general anaesthetic for her. We saw Mr Wall again
in May with the results of the scan which again reconfirmed
the diagnosis and the need for the operation, although
again there was good news, there was no evidence yet
of intracranial pressure (pressure within the brain
due to a constricted space to grow) which meant the
operation was not mega urgent. For us, once we knew
it needed to be done we just wanted to get on with it,
despite the thought of it scaring the hell out of us!
For Lucy’s sake we had a fun
filled summer, and she had a long spell without any
illnesses – at this time it seemed so hard to
believe she had this underlying serious health condition
that required major surgery.
  Her
operation was scheduled for the Thursday before the
bank holiday weekend in August 2005. We had been told
that we would have a difficult few days, and that Lucy
would have to go in for 2 or 3 three days before her
op to have a series of tests to ensure all the “t’s
were crossed” and that she was healthy enough
to undergo surgery. The morning arrived when we had
to go into hospital. Lucy didn’t really know what
she was really in for, as parents we were very apprehensive.
We met lots of people during that week, it was reassuring
that everything was being done so thoroughly, eye and
ear specialists, neuropsychologists, neurosurgeons,
anaesthetists, paediatricians, Mr Wall, nurse specialists
and so on……bloods were taken to ensure an
exact match could be made for the transfusion that would
have to be done during surgery – Lucy did not
like the needles!! We worried about anything and everything
that week. Lucy had a minor cough and cold which worried
the hell out of us, but to the doctors this was a minor
issue that could be dealt with, reassured, but still
concerned that the operation was still to go ahead.
The Paediatric Dr on the ward was superb with us that
week. We were fretting, big time!On the Wednesday afternoon
Mr Wall met with us to go through the consenting for
the operation process, which took about an hour. We
knew there were real risks of this surgery, but to hear
it from the surgeon who was undertaking the operation
was a shock and we found it difficult to remain objective
and remember all the questions we wanted to ask. The
risks and dangers were major and plentiful. Frankly
you can’t remove a persons skull and put it back
on a different way without there being serious risks
to health and life. The positive thing we clung on to
was that out of the 40 or so operations similar to Lucy’s
over the last ten years performed in oxford only one
had had a problem during surgery. Her
operation was scheduled for the Thursday before the
bank holiday weekend in August 2005. We had been told
that we would have a difficult few days, and that Lucy
would have to go in for 2 or 3 three days before her
op to have a series of tests to ensure all the “t’s
were crossed” and that she was healthy enough
to undergo surgery. The morning arrived when we had
to go into hospital. Lucy didn’t really know what
she was really in for, as parents we were very apprehensive.
We met lots of people during that week, it was reassuring
that everything was being done so thoroughly, eye and
ear specialists, neuropsychologists, neurosurgeons,
anaesthetists, paediatricians, Mr Wall, nurse specialists
and so on……bloods were taken to ensure an
exact match could be made for the transfusion that would
have to be done during surgery – Lucy did not
like the needles!! We worried about anything and everything
that week. Lucy had a minor cough and cold which worried
the hell out of us, but to the doctors this was a minor
issue that could be dealt with, reassured, but still
concerned that the operation was still to go ahead.
The Paediatric Dr on the ward was superb with us that
week. We were fretting, big time!On the Wednesday afternoon
Mr Wall met with us to go through the consenting for
the operation process, which took about an hour. We
knew there were real risks of this surgery, but to hear
it from the surgeon who was undertaking the operation
was a shock and we found it difficult to remain objective
and remember all the questions we wanted to ask. The
risks and dangers were major and plentiful. Frankly
you can’t remove a persons skull and put it back
on a different way without there being serious risks
to health and life. The positive thing we clung on to
was that out of the 40 or so operations similar to Lucy’s
over the last ten years performed in oxford only one
had had a problem during surgery.
  The
day of Lucy’s operation came, Lucy was third on
the list, which meant she was likely to be started about
1pm. The morning was difficult as she wasn’t able
to eat or drink anything all morning, she didn’t
understand and was distressed by being so hungry and
thirsty. We took her out for a walk around town to try
and get her to sleep – we bought her a soft Eeyore
which she instantly fell in love with. We went back
to the ward, and I walked her up and down the corridors
for what seemed like hours. Finally we got the call
at about 1.30pm. She was dressed in a little gown, which
swamped her little frame. Nic carried her the 5 minute
walk to the theatre block. We both went into the Anaesthetic
room with her and both struggled to keep our emotions
in tact when she finally stopped jerking and fighting
as the gas mask was put over her face to put her to
sleep. We were ushered quickly out of the room so that
they could get on with the job – it was pretty
hideous that experience. Not something you can really
forget easily. The
day of Lucy’s operation came, Lucy was third on
the list, which meant she was likely to be started about
1pm. The morning was difficult as she wasn’t able
to eat or drink anything all morning, she didn’t
understand and was distressed by being so hungry and
thirsty. We took her out for a walk around town to try
and get her to sleep – we bought her a soft Eeyore
which she instantly fell in love with. We went back
to the ward, and I walked her up and down the corridors
for what seemed like hours. Finally we got the call
at about 1.30pm. She was dressed in a little gown, which
swamped her little frame. Nic carried her the 5 minute
walk to the theatre block. We both went into the Anaesthetic
room with her and both struggled to keep our emotions
in tact when she finally stopped jerking and fighting
as the gas mask was put over her face to put her to
sleep. We were ushered quickly out of the room so that
they could get on with the job – it was pretty
hideous that experience. Not something you can really
forget easily.
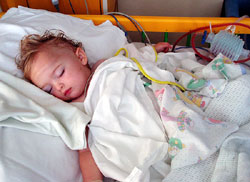
We wouldn’t see Lucy until about 7PM that evening,
and the afternoon was a bit of a blur. We wandered round
some shops aimlessly like zombies. It was horrible.
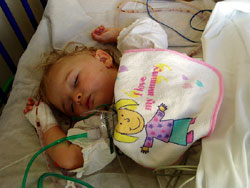
Feeling of total helplessness. When we saw Lucy that
evening she was completely asleep as she was being given
IV morphine as well as antibiotics and other drugs.
She would not be awake until the following day when
we would be able to hold her. (We had already been told
that we were not allowed to stay on the ward with her
that night as the staff would be too busy looking after
her). We met with Mr Wall who said that the operation
had gone totally according to plan and although having
needed a blood tranfusion, she had not lost a huge amount
of blood so he was very pleased. The relief of hearing
that was incredible.
We had so many people to ring
and to text about the news, we could feel the relief
in everybody. It meant a lot to us all that so many
people cared.
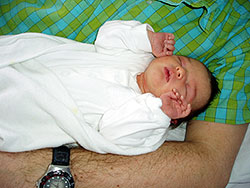
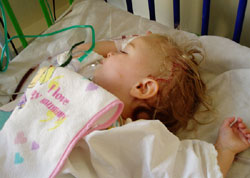
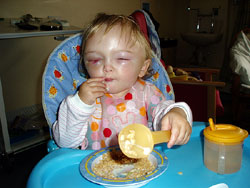 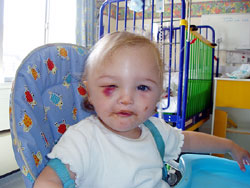 The
following day the full extent of the operation was clear,
Lucy looked in a bad way with a huge weeping scar from
ear to ear over the top of her head, and a huge black
eye. Two drains were sewn into her head, one round the
front of her head and one round the back. Strikingly,
her head seemed a completely different shape! Later
on in the day we were able to take her out of her cot
for the first time and we nursed her all day. As the
morphine was reduced she started to come back to life,
although still very groggy, she slept most of the day
interspersed with bouts of distress and crying. It was
a hard, distressing day. The staff on duty were always
there for reassurance and help whenever we needed them,
despite the stress of the situation, we felt in good
hands. That night was bad too and really was a low point
for me, we felt that Lucy wasn’t improving, but
in hindsight this was a ridiculous thought a day after
very major surgery! I sat up with Lucy rocking her till
the middle of the night whilst Nic tried to get some
sleep. I will never forget another parent (of a teenage
boy who was in being monitored for his epilepsy) coming
in to talk to me at about 2am with a large tumbler of
scotch – we shared our stories about our kids,
tried to have a laugh and enjoyed the booze. I will
never forget that moment, it was a small thing, but
it was so uplifting. Nic took over about 3am and I tried
to sleep – I have no idea how Nic kept going,
given that she was still in her first few weeks of pregnancy,
she was knackered and feeling nauseous. The
following day the full extent of the operation was clear,
Lucy looked in a bad way with a huge weeping scar from
ear to ear over the top of her head, and a huge black
eye. Two drains were sewn into her head, one round the
front of her head and one round the back. Strikingly,
her head seemed a completely different shape! Later
on in the day we were able to take her out of her cot
for the first time and we nursed her all day. As the
morphine was reduced she started to come back to life,
although still very groggy, she slept most of the day
interspersed with bouts of distress and crying. It was
a hard, distressing day. The staff on duty were always
there for reassurance and help whenever we needed them,
despite the stress of the situation, we felt in good
hands. That night was bad too and really was a low point
for me, we felt that Lucy wasn’t improving, but
in hindsight this was a ridiculous thought a day after
very major surgery! I sat up with Lucy rocking her till
the middle of the night whilst Nic tried to get some
sleep. I will never forget another parent (of a teenage
boy who was in being monitored for his epilepsy) coming
in to talk to me at about 2am with a large tumbler of
scotch – we shared our stories about our kids,
tried to have a laugh and enjoyed the booze. I will
never forget that moment, it was a small thing, but
it was so uplifting. Nic took over about 3am and I tried
to sleep – I have no idea how Nic kept going,
given that she was still in her first few weeks of pregnancy,
she was knackered and feeling nauseous.
 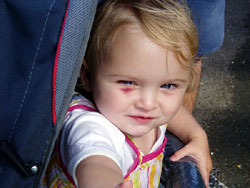 After
the difficult night the Saturday morning was a turning
point. Lucy awoke and started demanding food and drink
(for the first time since Wednesday lunchtime), we were
so relieved and proud that suddenly we had our little
girl back. She seemed to get stronger by the minute
from that moment. Saturday morning also saw the dreaded
time when the drains were due to be removed. I held
her while the nursing staff unpicked the stitches and
pulled out the drains – it was not pleasant and
Lucy found it distressing. We had been told to expect
serious swelling from that point on but that this was
a normal part of the healing process. By late afternoon
Lucy’s eyes were completely shut with severe swelling,
her head looked like it was going to burst. Lucy didn’t
seem to care, by this time she was toddling off down
the corridor to the play room with her grandparents
who had arrived earlier. It was wonderful to see her
getting back to normal. Over the next few days she continued
to improve and her head swelling gradually subsided. After
the difficult night the Saturday morning was a turning
point. Lucy awoke and started demanding food and drink
(for the first time since Wednesday lunchtime), we were
so relieved and proud that suddenly we had our little
girl back. She seemed to get stronger by the minute
from that moment. Saturday morning also saw the dreaded
time when the drains were due to be removed. I held
her while the nursing staff unpicked the stitches and
pulled out the drains – it was not pleasant and
Lucy found it distressing. We had been told to expect
serious swelling from that point on but that this was
a normal part of the healing process. By late afternoon
Lucy’s eyes were completely shut with severe swelling,
her head looked like it was going to burst. Lucy didn’t
seem to care, by this time she was toddling off down
the corridor to the play room with her grandparents
who had arrived earlier. It was wonderful to see her
getting back to normal. Over the next few days she continued
to improve and her head swelling gradually subsided.
We left hospital on the Monday afternoon
only 5 days after the operation – the speed of
recovery still amazes us to this day. We left hospital
with a list of do’s and don’ts and instructions
on how to care for the wound. If it scabbed we had to
remove them by scrubbing and the stitches had to be
removed. The scrubbing of the wound seemed counterintuitive
to us, Lucy’s head would be streaming with blood
and it clearly distressed her, and us for that matter.
However, we trusted the advice and did this diligently
morning and night. This process seemed to be endless,
but eventually over a period of weeks the scabs subsided
and the wound healed beautifully.
By and large things since have been
plain sailing in comparison, give or take the odd accident
and head knock (which always makes our hearts skip a
beat!). A year on Mr Wall is still pleased with progress,
as are we.
|